You may have heard the buzz around fasting and its powerful health benefits—but let’s face it, the idea of going days without food doesn’t exactly sound appealing or practical for most people. That’s where the ProLon Fasting Mimicking Diet comes in.
ProLon is a 5-day nutrition program designed to give you the benefits of a traditional fast—such as cellular rejuvenation, fat loss, and reduced inflammation—without actually going completely without food.
Developed by Dr. Valter Longo and backed by research from the USC Longevity Institute, this unique protocol mimics the effects of fasting while allowing you to eat specially formulated, plant-based meals.
WHAT EXACTLY IS A fasting mimicking diet?
Unlike intermittent fasting or water-only fasts, the ProLon diet allows you to consume a specific blend of nutrients that keeps your body in a fasting state while still receiving nourishment. Over five days, your body is gently guided into a fasting response, where it begins to use stored fat for energy and initiates cellular clean-up processes like autophagy—your body’s way of getting rid of old, damaged cells.
The meals are pre-packaged and provided in a convenient kit, including soups, nut bars, herbal teas, and supplements, with each day’s contents carefully calibrated for maximum benefit. The diet is low in protein and sugar, moderate in complex carbohydrates, and rich in healthy fats—enough to fuel you, but not enough to “wake up” your metabolic sensors that would otherwise break a fast.
WHAT ARE THE BENEFITS?
Clinical studies have shown a variety of potential benefits of the Fasting Mimicking Diet, including:
- Weight loss, particularly abdominal fat
- Improved metabolic markers, including blood glucose, cholesterol, and triglycerides
- Reduced inflammation
- Support for healthy aging and longevity
- Enhanced cellular regeneration
Some patients also report feeling more mentally clear and energized following the program, along with improved sleep and digestion.
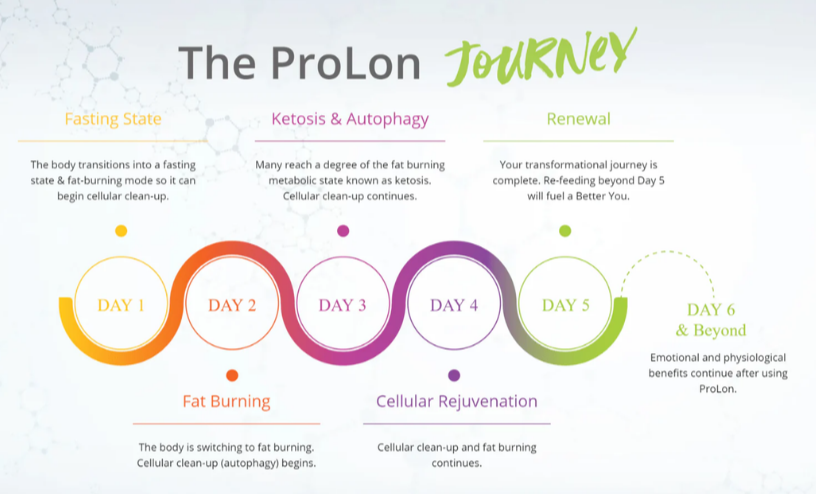
HOW DO YOU FOLLOW THE Prolon diet?
The ProLon program is incredibly easy to follow—everything you need for five days is included in the box:
- Day 1: About 1,100 calories to ease your body into fasting mode
- Days 2–5: Approximately 750–800 calories per day to maintain the fasting state
Each meal is clearly labeled by day and time (breakfast, lunch, dinner), and the kit includes herbal teas and an energy drink to support hydration and energy levels.
Many people choose to complete the ProLon FMD one 5-day cycle every three months for a year, followed by maintenance cycle of once a year. However, we tailor recommendations based on your individual needs and health history. Always check with a healthcare provider to see what’s appropriate for your health status and goals.
is it right for you?
The ProLon Fasting Mimicking Diet is not for everyone—pregnant or breastfeeding women, individuals with certain medical conditions, or those on specific medications should not use it without medical supervision.
If you’re interested in trying ProLon or learning whether this kind of fasting could be a helpful tool in your health journey, we’re here to help. We are currently carrying Prolon in the practice. Schedule a consultation to talk with our team and determine the best approach for your body’s unique needs.
To schedule an appointment with one of our certified Functional Medicine Physicians, please give us a call. We are excited to partner with you on your journey to optimize your health and wellness through personalized care tailored to your unique needs.
919.999.0831